
Focus on Wellness: Getting Your ZZZs

Strategies to help put common sleep obstacles to bed
Sixty percent of Americans have trouble sleeping, according to the National Sleep Foundation. For individuals with neuromuscular diseases, that number is likely higher, because disease-related factors, including limited mobility and respiratory problems, can make it difficult to achieve deep, restful sleep.
Research shows that proper sleep is important for maintaining physical and mental health. But if it’s your health that’s preventing you from getting a good night’s sleep, you might feel stuck. Fortunately, by identifying what’s keeping you up, you can develop strategies to put those sleep obstacles to bed.
Physical discomforts
Mark Eisenberg, 23, has Duchenne muscular dystrophy (DMD). Since his diagnosis at age 4, he has gone from sleeping on his stomach to lying on his back. “It’s easier to breathe and move,” Eisenberg says. “Gravity does all the work.”
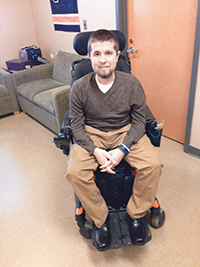
But being limited to one sleeping position raises its own challenges. If a limb begins hurting or an arm is twisted awkwardly, it can be difficult to adjust or turn. “I get in one position, and I kind of have to stay there,” he says.
Further complicating positioning issues are neurological ones. “Many individuals with neuromuscular conditions may have decreased sensation, so they can’t sense where their joints are in space,” says Kim Dohm, an occupational therapist with the MDA Care Center at the University of Missouri. “Maybe you need to move your foot an inch to the left, but you’re not even sure if it’s your foot that’s uncomfortable.”
Give them a rest: Comfortable bedding and an adjustable, low air-loss mattress can help prevent discomfort. For example, Eisenberg recently traded in a lumpy four-year-old mattress for a new adjustable model with special foam.
“There are fewer bumps and grooves to get stuck in,” he explains. “I can raise the bottom if I need to move my leg, or raise the top if I need to slide down on my pillow,” he says.
Sleep interruptions
During sleep, we often drift between sleep cycles, and even a good night’s sleep may include small awakenings. But when a sleep cycle is interrupted, it is harder to fall back asleep.
For individuals with neuromuscular diseases, positioning issues and pain can be common culprits of sleep interruption.
At his home in New Jersey, Eisenberg manages most nights with minimal interruption. But on the nights he does need help, the experience can be tedious. “Sometimes I’ll wake up because my body is in an awkward position or in lots of pain,” he says. “And it will require my mom rolling me over or propping me up for 20 minutes until the sensation disappears.”
Give them a rest: When an individual needs a caregiver’s assistance to turn, draw sheets can make the process smooth and quick. For even less disruption, consider a turning mattress that automatically shifts the sleeper periodically throughout the night to help change position and minimize the risk of developing pressure sores.
Environmental obstacles
According to the National Sleep Foundation, the optimal bedroom environment is cool, dark and quiet. But for some conditions, or as diseases progress, bulky or noisy equipment must be present in the bedroom.
“Many people have some device, like an oxygen concentrator or a BiPAP,” Dohm says. “And all that requires more equipment, more assistance and more time to accommodate.”
Give them a rest: Use a white noise machine, fan or air purifier to mask unwanted noise. No matter what your bedroom environment is, consider practicing meditation, which is a powerful tool for promoting relaxation. Eisenberg works with his respiratory therapist on breathing techniques. “By focusing on my breathing, I can allow the other disruptions to fade,” he says.
Shaila Wunderlich is a freelance journalist in St. Louis who has worked for a variety of magazines, journals and newspapers for nearly 20 years.
Sleep Assists
Accessory storage. Keep bedtime essentials close at hand. Simple Sheets’ Storage Pocket ($8.99) attaches to the side of the mattress.
Adjustable beds. Invacare’s Full-Electronic Homecare Bed ($1,768) raises electronically and has three layers of special foam for comfort and support. Assured Comfort Beds also makes adjustable beds with a high/low feature ($3,750 to $7,700) that can fit into most existing bed frames.
Grabbers. These long-handled helpers take the anxiety out of simple tasks like scratching an itch or moving a blanket. Duro-Med’s lightweight 32-inch Reacher Grabber ($9.67) has an ergonomic trigger handle and a magnetic strip for picking up metallic objects.
Respiratory aids. Provent’s tiny nasal device mimics the benefits of a CPAP machine without all the bulky equipment. Requires a prescription.
Smooth, clean bedding. Simple Sheets’ Velcro-adhering top sheet ($45.99 for a four-pack) keeps bed sheets smooth and is easy to change when dirty.
Supportive pillow. Contour Products’ CPAP Pillow 2.0 ($49.95) is shaped to avoid putting pressure on a breathing mask.
Turning bed. ProBed’s Freedom Bed automatically rotates sleepers who need assistance with turning and relieving pressure on different parts of the body. Contact ProBed directly to obtain pricing information.
Healthy Sleep Habits
Everybody needs good sleep habits. Optimize your sleep by following this advice from the National Sleep Foundation:
1. Stick to a schedule. Try to go to bed and wake up at the same time every day, even on weekends. This helps to regulate your body’s clock.
2. Practice a relaxing bedtime ritual. Having a relaxing routine right before bedtime helps separate your sleep time from activities that can cause excitement or stress.
3. Be active every day. Physical activity helps promote sleep, but avoid anything vigorous close to bedtime. Exercise circulates endorphins in the body, which may keep you awake.
4. Make your bedroom your sanctuary. Design your environment to establish the conditions you need for sleep. This includes keeping the temperature between 60 and 67 degrees, masking noises, and blocking out light and other distractions.
5. Sleep comfortably. Make sure your mattress and pillows provide the support and comfort you need.
Talk to Your MDA Care Center
Be sure to speak with your MDA Care Center team if you experience any sleep difficulties. They may be able to help tailor strategies to your needs.
Catch Your Breath
For individuals with neuromuscular diseases, nighttime respiratory problems can be responsible for sleep disturbances. Read Not Enough ZZZzzzs? to learn more about testing and treatment for sleep-breathing problems.
Editor's Note: Read the companion article in our Focus on Wellness series, Focus on Wellness: Get Moving, to learn about physical activity and how it may be easier to stay active with a neuromuscular disease than you think.
MDA Resource Center: We’re Here For You
Our trained specialists are here to provide one-on-one support for every part of your journey. Send a message below or call us at 1-833-ASK-MDA1 (1-833-275-6321). If you live outside the U.S., we may be able to connect you to muscular dystrophy groups in your area, but MDA programs are only available in the U.S.
Request Information