
Focus on Wellness: Get Moving

Physical activity is good for every body — and it may be easier to stay active with a neuromuscular disease than you think
Some individuals consider exercise a four-letter word, while others can’t seem to get enough. Whatever your feelings, the research shows that physical activity is good for everyone. Inactivity can lead to secondary health problems, such as high blood pressure and diabetes. A lack of exercise can quickly put on the pounds. Weakened muscles burdened with added weight is a double whammy.
There is no one-size-fits-all exercise prescription for people living with neuromuscular diseases. One person might be climbing mountains, while another needs assistance to climb into bed. The degree to which an individual can be active depends on a wide range of variables, even for those who have the same disease.
Whatever your abilities, incorporating physical activity into your life can help you manage your disease by maintaining flexibility, strength and mental fortitude. Before starting any physical activity or exercise program, consult with your MDA Care Center physician and physical therapist for guidance.
Break the barriers
Committing to a more active lifestyle can be challenging for individuals with neuromuscular diseases, especially for those with a new diagnosis or those who have not yet embraced exercising. A variety of potential obstacles can waylay the best intentions: lack of accessible facilities and equipment, cost, time or the need for someone else’s assistance.

Pennie Naylor, 60, has never considered herself athletic, but she always enjoyed walking. “Walking was my therapy. I would just walk and walk and solve my problems and the world’s problems,” says Naylor, who explains that Charcot-Marie-Tooth disease (CMT) has deteriorated the muscles in her hands and feet. “Walking one step for me is equal to someone else walking four or five,” she adds. “What few steps I have, I give to my dog.”
Now, Naylor rides a stationary bike twice a week. “It’s a replacement for walking. You can kind of get lost in it,” she says.
Do what you like
Staying active is a lifelong commitment. You’ll be more likely to stick with an exercise routine if it suits your abilities and your interests.
Owen Kent, 24, was tired of traditional physical therapy sessions. Kent has spinal muscular atrophy (SMA) and uses a power wheelchair. To start something new, he turned to his physical therapist at his local MDA Care Center, Tina Duong, who helped him locate an aquatic therapy program within a 10-minute drive of his home. For Kent, returning to the pool is motivating. As a child, he swam often and always enjoyed the water.
Duong, a physical therapist at Stanford University School of Medicine, tells her patients, “Focus on what you like to do, because exercising isn’t an easy thing to keep doing.”
To set yourself up for success, she advises talking with your medical team about the kinds of exercise you might be able to do. “Individuals need to be their own advocates and let their therapists know they want to maintain an active lifestyle that is feasible beyond visiting the [MDA Care Center],” says Duong.
Just move
Melissa Fox, a physical therapist at the MDA Care Center located at the University of Virginia, explains that when people continually sit, their muscles and tendons contract, which can cause pain. To avoid this problem, it is imperative to move and explore assistive technology like a mobile stander or standing wheelchair.
Of course, being active doesn’t mean you have to do 100 pushups or spend hours sweating at a gym. According to Fox, anything that gets you moving can count as exercise, even active video games, such as tennis or race car driving.
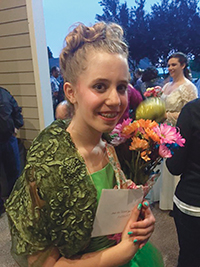
For 13-year-old Natalie Dion, mitochondrial myopathy limits her activity level and requires constant monitoring between exertion and resting, explains her mom, Nicole. The disease weakens muscles and causes fatigue.
At school, Natalie plays on a volleyball team, which is good for her coordination. The coach allows her to skip the pregame running and has her play in short bursts. “If Natalie does too much, she can be down for days,” Nicole says.
Keeping her daughter active is important for her health, and Nicole sneaks in a variety of physical activities to make exercise fun. The family frequently splashes in the pool or turns on music and dances around their house. Outside, Natalie enjoys bouncing for five or 10 minutes at a time on her trampoline. Indoors, Natalie uses a jump rope, climbs the stairs or does airplane stretches on a large exercise ball. Last year, loom bracelets were the rage, and Natalie worked on her finger dexterity while making rubber band jewelry.
Figuring out how much Natalie can physically do varies from day to day. “It’s all about finding the balance and adjusting accordingly,” says Nicole.
Practice moderation
Most neuromuscular diseases are progressive and frequently cause fatigue. Performing daily tasks such as dressing, gardening and housework may be an adequate amount of physical activity for some.
“We teach people a lot about what we call ‘energy conservation,’ which is how to manage your energy throughout the course of the day,” says Fox. “It’s not going to be the same amount you had before your diagnosis or the same amount as an average person.”
Think about what your day entails and pace yourself. For example, don’t spend the morning at the gym if you are scheduled to attend a party that evening. Loading your dishwasher might be a more productive way to expend energy than lifting weights.
Gauging how much you can do means listening to your body. If you feel worse after an activity, you might be overworking your muscles. Individuals with neuromuscular diseases should not overexercise. “For example, if you do too many squats, you’re more likely to fall later in the day because your legs are tired,” says Fox.
Be adaptable
When you’re ready to be more active, remember to start small and build up gradually. Try new activities to keep your routine fun. And most importantly, continually re-assess your fitness goals with the help of your physician to make accommodations for your changing body.
Four years ago, Naylor joined a Pilates class and credits her twice-weekly sessions with strengthening her core and improving her balance. “Pilates is phenomenal. I’m in the beginners’ class, and I’ll always be in the beginners’ class. I don’t progress like other people do, and that’s OK,” says Naylor.
“The key is to adapt,” she says. “I don’t look at what I can’t do anymore. Instead, I look at what I’m able to do.”
Barbara Twardowski has Charcot-Marie-Tooth (CMT) disease and uses a power wheelchair. Jim, her husband, is a registered nurse. Both have degrees in journalism. They live in Louisiana and write about accessible travel, health and lifestyle, and related issues.
Join the Fitness Community
“Most of us get a lot of joy out of going out,” says Tina Duong, a physical therapist at the MDA Care Center located at the Stanford University School of Medicine. “Finding a group exercise or activity that works for you could be fun.”
Follow these five tips to find exercise classes or activities that meet your unique needs:
• Talk with your local MDA office to find community resources. Some hospitals, rehabilitation facilities and senior centers offer wellness programs or classes designed for people with disabilities or chronic medical conditions.
• Join support groups and ask other members what they do to stay active.
• Search the National Center on Health, Physical Activity and Disability’s website for programs in your state.
• Find adaptive fitness programs through Disabled Sports USA, which has information on 45 adaptive sports, from archery to yoga.
• Attend one of the eight Abilities Expos to learn about adaptive sports and inclusive recreation in the region.
Stay Motivated
Everyone occasionally needs a carrot to keep plugging away at an exercise program. Use these tips to stay active.
• Use the buddy system. Knowing someone is waiting for you at yoga class can be a powerful incentive.
• Write how you feel after exercising in a fitness journal. Read this journal when enthusiasm is waning.
• Reward yourself with a new exercise outfit or piece of equipment. How about a waterproof iPod Shuffle for the pool?
• Try something different. Join a new class or buy a video game that gets you moving.
• Listen to an audiobook only when you exercise. You’ll be eager to hear the next chapter.
Editor's note: In addition to staying active, getting a good night's sleep is important. Read Focus on Wellness: Getting Your ZZZs to learn about strategies that can put common sleep obstacles to bed.
MDA Resource Center: We’re Here For You
Our trained specialists are here to provide one-on-one support for every part of your journey. Send a message below or call us at 1-833-ASK-MDA1 (1-833-275-6321). If you live outside the U.S., we may be able to connect you to muscular dystrophy groups in your area, but MDA programs are only available in the U.S.
Request Information