
Scoliosis Surgery: Before and After

Staying ahead of the curve
You hope it won't be necessary, but it often is: surgery to correct scoliosis, a lateral (side-to-side) curvature of the spine. Scoliosis can occur in almost any neuromuscular condition in which back muscles, which normally keep the spine straight, weaken, but it's particularly common in Duchenne muscular dystrophy (DMD) and spinal muscular atrophy (SMA).
 In DMD, a boy often rapidly develops scoliosis in adolescence, usually after he's been using a wheelchair full time for a while. In SMA, a slowly progressing scoliosis often has its onset in childhood. The treatments for scoliosis in these two diseases may be slightly different (for instance, bracing is hardly ever used in DMD but is sometimes used to stave off surgery for a while in SMA), but the underlying causes and basic approaches are much the same.
In DMD, a boy often rapidly develops scoliosis in adolescence, usually after he's been using a wheelchair full time for a while. In SMA, a slowly progressing scoliosis often has its onset in childhood. The treatments for scoliosis in these two diseases may be slightly different (for instance, bracing is hardly ever used in DMD but is sometimes used to stave off surgery for a while in SMA), but the underlying causes and basic approaches are much the same.
The experience of Jason Abramowitz, now 17, and his mother, Adele, of Columbia, Md., is fairly typical for a young man with DMD whose scoliosis has reached the point of requiring surgery.
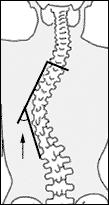
As they begin their story last fall, 16-year-old Jason's spinal fusion surgery (see "Medical Perspective,") is scheduled for Nov. 30 with Nancy Miller, an orthopedic surgeon at Johns Hopkins Hospital in nearby Baltimore. X-rays have shown that Jason's scoliotic curve is progressing rapidly. According to Adele, it's gone from 20 degrees in April to 35 degrees in August to 40 in November (see "Measuring the Curve" section below).
Adele and Jason had hoped to have the surgery performed over the summer, but insurance matters delayed the procedure, and now treatment is becoming urgent.
Nov. 12, 2001 — pre-surgery questions: Adele
What we're wondering now is, what is life going to be after the surgery? We're going in on the 20th to talk to the surgeon and ask questions.
I gather there will be changes in what Jason is physically able to do. Jason is an avid online gamer, with six or seven screen names, so my big concern is, how soon can he get back in front of the computer after the surgery?
 Nov. 26, 2001
Nov. 26, 2001
In talking with Dr. Miller, it seems Jason's going to be pretty much restricted to bed when he gets home, with initially just two hours a day sitting up in the chair. As he progresses and improves, that will increase. Right now, Jason's plans are to beat the record on getting from surgery back to school.
I'll say that Jason has responded very well to anesthesia in the past. He had tendon release surgery on his heel cords and hips, and as they were wheeling him into recovery, he opened his eyes and said, "I'm not throwing up, so can I have pizza now?"
But then he was only out for about 45 minutes, and Dr. Miller says this surgery is about eight hours.
Jason has been going to a cardiologist for about four years to get routine echocardiograms. We just got a great report back. So far the disease has had no impact at all on his heart.(Severe cardiac muscle deterioration — cardiomyopathy — may make a surgeon reluctant to perform the operation, as can severe respiratory muscle deterioration.)
The hardest part is that he'll be away from the computer for a while. Wheelchair football season has ended, and he was able to play the entire season, so at least he can't say he missed football.
Right now, the plan is that he'll be transferred in about a week's time (after the surgery) to Mount Washington Pediatric Hospital, where he'll be an inpatient for his rehabilitation. He might be there as long as a month or so.
 Mount Washington Pediatric Hospital, in Baltimore and two other Maryland locations, specializes in long-term and rehabilitative care of children and infants. Jason ultimately stayed at Johns Hopkins from Nov. 30 to Dec. 7 and at Mount Washington from Dec. 7 to 14, a much shorter time than expected.
Mount Washington Pediatric Hospital, in Baltimore and two other Maryland locations, specializes in long-term and rehabilitative care of children and infants. Jason ultimately stayed at Johns Hopkins from Nov. 30 to Dec. 7 and at Mount Washington from Dec. 7 to 14, a much shorter time than expected.
Once he's released from the rehab hospital, when he comes home, there's going to be therapy at home, because he'll have to learn how to do everything again — transfer, shower, dress, etc. If he's no longer able to do something a particular way, then he'll have to learn how to do it another way. We'll have therapists come to the house.
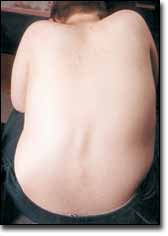
A lot of these young men use the curve in their spine to do things — to get their arms up, to wipe their face. He'll lose that ability.
When he goes to rehab, these people will have no idea what he usually does. They will never have seen him prior to the surgery.
They may look at him and not realize what he could do. This video (a video Adele is making of Jason's activities) is a good tool for going into rehab. They can see the old body mechanics and the new body mechanics. They can see how to translate what the body is able to do into getting back function. He'll never get back 100 percent; that much is a given. But we'll try to get back as much as we can.
The spinal curvature often allows a person with weakness and scoliosis to lean to one side and downward in order to bring his hand to his mouth or face, a movement necessary for eating and drinking. Many with DMD can also lean from side to side to relieve pressure on the buttocks while sitting. These functions are often lost when the spine is straightened and immobilized by fusion surgery. A video of how the person accomplished things before surgery can be helpful to rehabilitation professionals afterwards.
Insurance, blood donation and school adjustment
The other thing we have to deal with is insurance. We have to start implementing the changes in equipment now. The only thing I have done in that regard is to find out whether Mount Washington is covered for both inpatient and outpatient services, and it is. But I'm going nuts because I just found out on Tuesday that the doctor wants the pre-op blood work done at Hopkins.
We were hoping that this surgery could be done over the summer, but we had issues and more issues with the insurance company. They had me take him to someplace where they had probably not seen a young man with Duchenne dystrophy. They were not able at that place to do the X-ray the way it's done at Hopkins. (These X-rays had to be discarded.)
It's bloody surgery, so we did blood donations beforehand. I had it arranged so that they would get a unit from Jason, and I and my older brother and sister all made arrangements to donate blood toward the surgery. As it turned out, they weren't able to take blood from Jason because he's got small veins, so the needle they needed to use to take blood was much bigger than his veins were.
It's often recommended that children about to undergo scoliosis surgery donate their own blood prior to the procedure. Sometimes family members and friends can also become "directed donors" for a particular patient, although it should be noted that relatives and friends will be asked personal questions about their lifestyles and health histories and that their blood will be screened in the same way as any other donor's blood.
Ask the physician in charge and the blood bank about local blood donation procedures at least several weeks before the surgery is scheduled to be performed.
Once he's well enough we'll have a much better idea of when he's going to return to school. We need to have the school re-evaluate him for physical therapy, assistive technology, etc. He'll lose some of the functions that everybody in school has been taking for granted. Things like how he can sit at a desk, and will the desk there be sufficient for him now that he can no longer slouch over when he does his writing? The school has to do all those evaluations. They'll do them, but whether they'll do them adequately and in a timely fashion is another question.
He'll get some home schooling, but the county will provide only six hours a week compared to the six hours a day that he gets now at school, so there are some things that Jason is just not going to get.
When he does return to school, I want him to be able to jump in and pick up where he left off. If we have to wait for furniture and equipment, there will be that many more weeks before he can function in school and get decent grades, and this is an important year for him in school. (Jason was in the 11th grade.)
Jason is usually pretty "up," but we have our moments. Surgery is really going to throw him for a loop. How he responds, physically and emotionally, is virgin territory for us.
Nov. 26, 2001 — Jason's pre-surgery feelings
Jason is ambivalent about the surgery, saying he has "yeses and nos" about it.
The yeses are that it will give me a better posture. I'll look better because I won't be crooked. I'll be able to sit up straight and get less backache. I get backaches now. The no would be that I won't have that much movement.
I had tendon release surgery when I was about 9 or 10, and it helped me a lot. It sort of did help me walk longer.
Dec. 24, 2001 — after surgery: Adele
We've been home for a little more than a week now. Jason is doing better. He still has a lot of pain, but he's getting better every week. On Wednesday, we'll have occupational therapy here to figure out what kind of equipment, if any, will help Jason do many of the things that he can't do right now.
Jan. 8, 2002
Jason's incision is coming along just fine. PT is going OK now, and I had my first meeting with the new occupational therapist today. On Tuesday, Jan. 15, we go back to see Dr. Miller.
As for occupational therapy, most of what they'll be doing with Jason is probably going to have to wait until he gets his new wheelchair. They'll help in getting the new chair.
Jan. 10, 2002 — therapy and school
Jason is still progressing. The new occupational therapist is due here tomorrow, and the wheelchair person is also due then. We're still waiting for Jason's new chair. We have a temporary chair, but it's too high. We can't get it under the computer table or the kitchen table. The van is a problem also. For now, we'll modify his old chair.
Also, there are issues with his desk — and the bus for school needs to be resolved.
Jason's hours at school were changed after the surgery, necessitating a new bus schedule — not easy to arrange.
 After scoliosis surgery, people are usually a few inches taller, because the spine has been straightened, and, if a new wheelchair is required, it may seat the person higher. Both these changes mean more headroom is needed in a vehicle. Desks, computer work stations and tables may also need to be modified.
After scoliosis surgery, people are usually a few inches taller, because the spine has been straightened, and, if a new wheelchair is required, it may seat the person higher. Both these changes mean more headroom is needed in a vehicle. Desks, computer work stations and tables may also need to be modified.
We've had to fight with the insurance company to get the therapists that we wanted to work with. One OT didn't think Jason could accomplish his goals. This OT that we've engaged now is more familiar with Duchenne dystrophy, and she's more aggressive.
Also, he's more limber now with the physical therapy.
The arm support will be here tomorrow. (Its arrival was delayed.) He can't eat now without something like this. He'll need it to get his hand to his face.
We thought Jason would be back at school at the end of this month or the beginning of February, but now we're not so sure. (Jason started home schooling at the end of January and was able to return to school at the end of February. In May, he was attending school for partial days, with home schooling as a supplement.)
His medical progress has been good. Monday, he was able to sit up unsupported. He's doing more than was expected, and that has helped his outlook a bit. But he has less independence since the surgery, and it's going to be hard work to bring it back. He'll regain some of his independence, but he's a young man and he's impatient. He's been having some depression, because he's lost the independence that he had.
In contrast to corrective spinal surgery in the general population, such surgery in adolescents with neuromuscular disease generally leads to a loss, rather than a gain, of function, at least temporarily and sometimes permanently. In return there are other gains, such as avoiding a "pretzel type" deformity and possibly sustaining pulmonary function, although this last point is controversial. Honest exploration of this with a teenager may be advisable.
April 2002 — a new wheelchair
In the spring, Jason and Adele went to see John Bach, a physical medicine and rehabilitation specialist who co-directs the MDA clinic at the University of Medicine and Dentistry in Newark, N.J. Bach specializes in maintaining respiratory health in children and adults with neuromuscular diseases.
April 19, 2002
Our visits with Dr. Bach and Dr. Miller went well. Both are very pleased with Jason's current condition and his overall good health.
The new chair is coming along a piece at a time. We have a new seat to try, but we had to make a few adjustments to the chair, so the new seat doesn't fit yet. We're hoping to have a seat and a back in place some time next week. Then they have to attach the mobile arm support. At that time, physical therapist Lee Winemiller will be back to help Jason learn to use it.
Thursday is Jason's birthday. He'll be 17.
May 1, 2002 — reflections and surprises
Adele was asked to reflect on having had the scoliosis surgery performed and on possible advice to other families.
I'm glad we had the surgery done. I know what the consequences would have been if he hadn't had it done. The way the scoliosis was progressing, quite rapidly, it would have been a matter of maybe two years before he would have been in such discomfort that it would have made his life very, very difficult.
I want him to be able to sit in his wheelchair and sleep in a bed without all sorts of special arrangements and for him to be as healthy and as normal-looking as possible.
But there were some surprises, some things I didn't think of.
 One thing was in trying to get the equipment.
One thing was in trying to get the equipment.
I was so into Jason's care that I sort of left getting the new equipment up to other people. Normally, I would have made calls once a week to see what was going on. I should have taken a more active role. After I made a few phone calls, when I finally got involved, things moved along.
Insurance
I have a case manager for Jason through the insurance company, but companies have different criteria for being part of the case management system, and sometimes they only give it to you if you're going to go into the hospital. Not everyone routinely has a case manager, but if you can get one through your insurance company, I would suggest it in a heartbeat.
Then there were a couple of unexpected medical problems. The wound opened up, and, although Jason wasn't in a lot more pain than anticipated, it was a longer duration of pain.(The incision eventually healed satisfactorily, and the pain resolved over time.)
School
With the school, I think the biggest thing is to give the school plenty of information, plenty of notification, and make suggestions. I've been talking to the school since the first day Jason went to school as a junior. Even before that, when the scoliosis was moving and we were waiting to schedule surgery, I kept the school informed of his condition.
They did have plenty of time to think about it and to keep it in the backs of their minds so that when it did happen, it went extremely smoothly and they provided services that he needed.
I had thought that if the surgery went OK and if we were satisfied with the rehab, then basically it was just a healing process. It didn't all go as perfectly as I had envisioned. But in talking with other parents and with the doctors, Jason's progress was excellent.
May 2002 — Jason's post-surgery thoughts
I feel all right. I just have a few pains.
The worst parts?
At the rehabilitation hospital, when I had to do physical therapy. It was pretty painful.
And I had to get used to sitting in the wheelchair starting a week after surgery, and there was a little more pain than I had expected.
School is a little more difficult because I get tired a little more easily.
Was it all worth it?
Yes. I can sit better. I have less backache.
MDA Resource Center: We’re Here For You
Our trained specialists are here to provide one-on-one support for every part of your journey. Send a message below or call us at 1-833-ASK-MDA1 (1-833-275-6321). If you live outside the U.S., we may be able to connect you to muscular dystrophy groups in your area, but MDA programs are only available in the U.S.
Request Information