Facioscapulohumeral Muscular Dystrophy (FSHD)
Medical Management
There is currently no cure or disease-specific treatment for facioscapulohumeral muscular dystrophy (FSHD). Care focuses on managing symptoms, maintaining function, and supporting quality of life.
Pain and symptom management
Some individuals experience musculoskeletal pain or fatigue. Medications may be recommended by a doctor to help manage discomfort, including nonsteroidal anti-inflammatory drugs (NSAIDs) and, in some cases, medications such as antidepressants or antiepileptics for chronic pain. Supportive approaches such as stretching, positioning, or heat therapy may also be helpful.
Rehabilitation and supportive care
Physical and occupational therapy can help maintain mobility, improve posture, and support daily activities. Speech therapy may be helpful in select cases.
Assistive devices are commonly used to support weakened muscles and improve safety and independence. These may include:
- Bracing, such as ankle-foot orthoses (AFOs), to help with walking and reduce the risk of falls
- Postural supports to improve alignment and reduce strain
- Other adaptive equipment as needed for daily activities
Surgical options
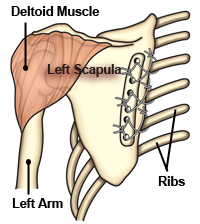
In some individuals, a procedure called scapular fixation (or scapulothoracic fusion) may improve arm function by stabilizing the shoulder blade. This option is typically considered on an individual basis and performed by surgeons experienced with FSHD.
Exercise
Research and clinical experience suggest that low- to moderate-intensity exercise may be safe for many people with FSHD and can help support overall health and function. Programs are often tailored to the individual and focus on maintaining strength in less-affected muscles while avoiding overexertion.
Monitoring and multidisciplinary care
FSHD is not usually associated with heart involvement, but some individuals may develop breathing or other complications, particularly in more severe cases. Regular follow-up with healthcare providers familiar with neuromuscular conditions can help monitor and address changing needs over time.
Nutrition
There is no specific diet proven to treat FSHD. General nutrition and, when needed, guidance on maintaining a healthy weight and addressing swallowing or metabolic concerns may be part of supportive care.
FSH Care Guidelines for Clinicians (Downloadable PDF)
FSH Care Guidelines for Patients and Families (Downloadable PDF)
Additional reading
- Tawil R et al.; Guideline Development, Dissemination, and Implementation Subcommittee of the American Academy of Neurology (AAN); Practice Issues Review Panel of the American Association of Neuromuscular & Electrodiagnostic Medicine (AANEM). Evidence-based guideline summary: Evaluation, diagnosis, and management of facioscapulohumeral muscular dystrophy: Report of the Guideline Development, Dissemination, and Implementation Subcommittee of the AAN and the Practice Issues Review Panel of the AANEM. Neurology. 2015 Jul 28;85(4):357-64. doi: 10.1212/WNL.0000000000001783.
Last reviewed April 2026.

