
Understanding Heel Cord Surgery

Cutting the cord
Tom Baker, 14, is the second child of Harold and JoAnn Baker of Dover, Ohio. When he was a small boy, the family noticed that he walked "funny," certainly not like their first child, Jessica, now 18, or their youngest, Lisa, 11.
Still, doctors weren't terribly concerned until the Bakers took Tom for his kindergarten physical. "The doctor noticed that he exhibited the Gowers' sign," JoAnn recalls, referring to the way children with leg muscle weakness use their arms to brace themselves when getting up from the floor.
A blood test to measure creatine kinase — which leaks out of damaged muscle cells in muscular dystrophy — quickly followed. "It was 16,000 [much higher than normal], and that pretty much clinched it," JoAnn says. In a stroke of what seemed like good luck in the midst of bad, the Bakers' pediatrician told them about a famous specialist in neuromuscular disorders, Jerry Mendell, who worked not too far away at Ohio State University Medical Center in Columbus.
There, in 1993, a biopsy confirmed the suspected diagnosis — Duchenne muscular dystrophy (DMD). Almost immediately, the Bakers enrolled Tom in a study of a corticosteroid (prednisone-related) drug. Unfortunately, JoAnn relates, the sponsoring pharmaceutical company abandoned the study. But Tom has remained on the medication ever since, a factor that may have helped him preserve more strength than expected in a child with a clear DMD diagnosis.
Slowing down
This summer, Tom and his parents were presented with a dilemma. "He's slowed down some," JoAnn said shortly before school was out, when Tom was still able to ride his bike (though not uphill much), ride a skateboard (though mostly in a sitting position), and keep up with his classmates (though he had recently stopped taking gym classes).
Walking was getting tougher, even though he didn't have any spinal curvature (common in boys with DMD as the disease progresses). His heart and respiratory function appeared good, and his thigh muscles seemed strong enough to support his weight fairly well.
A major problem appeared to be Tom's feet. His left Achilles tendon, a fibrous band also called a heel cord that anchors the muscles at the back of the lower leg to the heel bone, seemed to be tight and taut, causing the teen-ager to walk with his left foot "clear up on his toe." The right tendon was tight, too, but he could still get his right foot down flat, with effort.
Like many boys with DMD, Tom was wearing ankle-straightening splints at night, but these didn't seem to be keeping his feet straight.
His parents wondered: Would Tom soon need a wheelchair? Or was there a way to postpone that step?
Considering surgery
The Bakers turned again to the MDA clinic at Ohio State, consulting with John Kissel, the clinic's co-director, and Wendy King, a physical therapist who has followed Tom's progress since he first came to OSU in 1993.
They asked what could be done about Tom's toe-walking and inability to put his heels down. Could his feet be surgically straightened? It seemed a simple enough solution, but, as the Bakers were to learn, there are lots of questions about the procedure.
Known as heel cord tenotomy, heel cord release or Achilles tendon release, the procedure has come in and out of favor in DMD treatment over the years. (It's used in some other conditions, including strokes and cerebral palsy, and in the congenital muscular dystrophies. It's sometimes done in Becker MD and occasionally in spinal muscular atrophy.)
When performed at the right time on the right youngster with DMD, heel cord release can probably prolong walking for at least a couple of years, but studies are hard to interpret. In most investigations, the procedure has been combined with other interventions — additional surgery, physical therapy, splinting at night and/or corticosteroid medications. Studies don't generally separate the effects of these various treatments from one another.
One thing, however, seems clear: Cutting the heel cords at the wrong time on the wrong person can prematurely end walking.
Contractures and toe-walking
In years past, when a boy with DMD had trouble flattening his foot, parents and physicians would assume the problem resulted only from a heel cord (Achilles tendon) that was abnormally stiff and contracted. They often decided that cutting this cord would at least temporarily solve the problem. But often it didn't help, and it sometimes made matters worse.
What experts now know is that a tight heel cord can result partly from a contracture (a joint pulled into an abnormal position because the tissue around it shrinks and hardens) and partly from the child's efforts to balance himself in the face of increasing leg weakness.
The two processes are related: Once a child forms the habit of walking up on his toes to help him balance, the development of contractures (a usual part of DMD) is hastened. Holding the joint in an abnormal position for much of the day aids the shrinkage of soft tissues around the joint. The challenge is to separate the harmful contracture from a helpful one encouraged by the child's toe-walking.
Walking on the toes, though it looks awkward to observers, can actually help a child support his weight, by increasing the stability of the knee, physical therapist King explains. Pointing the foot downward makes the knee a little more stable. Releasing the tendon that helps the child do that may cause him to lose that benefit and may even prematurely end his walking ability.
Still, such surgery is warranted in some cases. "When it clearly seems indicated is when the degree of contracture development is outstripping the weakness or when contractures are having a role in destabilizing their gait," Kissel says.
Tom Baker, to the expert eyes of Kissel and King, seemed the ideal candidate for heel cord surgery. The next step was to suggest the ideal surgeon — in their view, Irwin M. Siegel.
Understanding mechanics
Irwin Siegel is an orthopedic surgeon whose interest in tendon releases and bracing to prolong walking in children with muscular dystrophy extends back more than three decades. Siegel co-directs the MDA clinic at Rush-Presbyterian-St. Luke's Medical Center in Chicago, where he's a seasoned evaluator of when surgery should — and shouldn't — be undertaken.
He's the first to admit that heel cord tenotomy in muscular dystrophy is an operation with a mixed
reputation. In the early days of enthusiasm for the procedure, he says, "people saw heel cord contracture and cut the heel cord, and kids never walked again." The important step here, he says, is what he calls "staging" of the patient — determining the right time for the surgery and whether it's likely to benefit the patient.
The indication for heel cord surgery, or any surgery, he says, is "whether it will help. The mere fact that you can do the operation is no indication."
Siegel agrees with Kissel and King that, in people with weak upper leg muscles, "the knee will help you if you come down on your toes instead of your heels." Heel cord contractures can be part of this effort.
"The heel cord contracture should be encouraged if it's aiding weak upper leg muscles and helping the person extend the knee," Siegel notes. "But it can become an inhibitor of standing and walking."
Understanding the biomechanics, he says, is crucial. "When the time comes, the compensatory mechanism is a problem, and the contractures have to be released," Siegel says. Recognizing this time, he says, is a matter of clinical judgment, made on a case-by-case basis, although there are functional tests that can guide a physician.
In general, he says, the right time to do heel cord surgery in DMD is when the child is having considerable trouble standing and walking, with independent walking imminently threatened, but before he begins using a wheelchair.
In Siegel's experience, once a boy is using a wheelchair extensively, it's all but impossible for him to regain the ability to walk. (Not all investigators agree with this. In one large study published in 1993, extensive surgery for release of multiple contractures, combined with bracing and use of a walker, allowed continued walking even in boys who had previously stopped.)
Before deciding on a surgical procedure, Siegel also takes into account whether the patient's cardiac and respiratory status are adequate for him to withstand anesthesia.
To guard against the small possibility of adverse reactions to anesthesia that are slightly more common in people with neuromuscular disorders, Siegel makes sure the surgical team is fully prepared with the right kinds of anesthetic agents. The team should also have on hand dantrolene (Dantrium), a medication to counteract an adverse reaction called malignant hyperthermia.
Casting, bracing — and very little resting
On June 5, Siegel performed a procedure called percutaneous tenotomy on both of Tom Baker's feet. He made a small stab wound in each heel to cut the tendon, rather than laying open the skin with a traditional incision. In this procedure, bleeding is insignificant, Siegel says; there are no sutures and virtually no surgical wound.
"All the complications of wounds are avoided, and the patient can stand and walk by the next day," Siegel says.
Siegel emphasizes that it's crucial "not to put the patient to bed." Bed rest, he says, results in rapid loss of strength in people with muscular dystrophy. In fact, he prefers that his patients stand and walk the day of surgery.
Before Tom awakened from the anesthesia, lower-leg casts were applied to keep his feet in their newly straightened position. Cloth "cast shoes" were attached to the casts for walking.
These casts, in Siegel's program, are temporarily removed so the boy can be fitted for braces about a week to 10 days later. They're then put back on for another week to 10 days, at which point the braces should be ready and are substituted for the casts.
Siegel prescribes brace wearing day and night for six weeks after heel cord surgery. Then, they need not be worn at night.
The Achilles tendons, Siegel explains, will grow back together, but the surgery has lengthened them and thus prevented them from interfering with walking in braces. In youngsters with adequate strength in the four-part muscle at the front of the thigh (quadriceps), such as Tom Baker has, lower-leg braces are sufficient to allow walking. These are commonly called AFOs, orankle-foot orthoses.
For those with weaker quadriceps, Siegel prescribes long-leg braces, or KAFOs (knee-ankle-foot orthoses).
Uncertainties remain
Not all physicians and physical therapists agree about heel cord releases. Some don't recommend them at all, citing the temporary nature of the correction in a progressive disease, the risk of interfering with walking ability, the apparently similar effectiveness of corticosteroid medications in prolonging walking, surgical risks, and the less than graceful gait provided by AFOs or KAFOs.
Families can have similar objections to surgery. And boys with DMD, as they reach their teen years, may find the prospect of zipping around school in a power wheelchair more attractive than labored ambulation with braces.
Some experts recommend heel cord tenotomy only as part of a larger surgical procedure, such as transferring a tendon from the back to the front of the foot (tendon transfer procedure) so the child can better lift his foot off the ground; or as part of a "triple release" procedure, in which contracted tissue at the hips, knees and ankles is released at the same time.
Some surgeons, such as Neil Green at Vanderbilt University Medical Center in Nashville, Tenn., object to heel cord tenotomies without simultaneous releases in the upper leg. Green, director of the Pediatric Orthopaedic Section at Vanderbilt, has been associated with the MDA clinic at Vanderbilt for many years.
"Heel cord lengthening, if it's done, must be done in conjunction with other muscle releases about the hips to allow the legs to be straightened enough to be put into braces," Green says. "It should be part of an overall program to decrease contractures of the hips, knees and ankles at the same time. If someone operates on a child with muscular dystrophy and does nothing but lengthen the heel cords, the child will stop walking, almost certainly."
Kissel says he understands such objections to isolated heel cord tenotomies but he's skeptical of rules applied to everyone.
"Clearly, there are boys that can do well just getting the ankles released. Some boys get such severe ankle contractures, while some get iliotibial band contractures," he says, referring to a band of fibrous tissue that goes from the hip down the side of the leg and can cause problems when it tightens.
"There are boys in whom one type of surgery is indicated."
Back to his routine
As for Tom, he's glad the surgery is behind him but not sorry to have had it done.
"I think it was worth it," he said five weeks after the procedure. Following a rocky first week requiring pain medication and then a few weeks of boredom and frustration, he resumed his former level of activity.
Tom's father is glad, too. "He was walking so crooked before that it was hurting his side. It was like having a big block under your foot; everything was misaligned. That's stopped now," Harold Baker said at the five-week point.
By the second week in July, Tom was back swimming, camping with his family, playing with his dog Midnight and cat O.C. (Orange Cat), and watching his sister Lisa play softball. He's also been building a motorized cart from a wagon and spare parts.
"I'm walking pretty good now. I'm not limping anymore," he said. The pain had almost disappeared.
Is walking worth it?
One of the debated points about heel cord surgery is whether extending the ability to walk is worth the surgical risk. Some argue that the past decade has brought a degree of mobility to people with neuromuscular impairments undreamed of in earlier times.
"Wheelchair" now refers to a powerful electronic vehicle that can zip around schools and malls, carrying books and packages and impressing friends. These high-tech conveyances offer much more freedom than yesterday's wheelchairs.
But, as glamorous and empowering as today's wheels may be, they still subject their drivers to the hazards of immobility almost as much as did the wheelchairs of yesterday.
Proponents of techniques to prolong walking in DMD point out that, once no longer upright and walking, the human body quickly acquires an array of physiologic problems. Siegel points to osteoporosis (bone loss); rapid deterioration of remaining muscle strength; enhanced progression of contractures, including spinal contractures leading to curvatures; weight gain; metabolic changes; constipation; fluid retention; and cardiac and respiratory complications. It's best to postpone these as long as possible, he says.
"Standing and walking are gifts," Siegel says, gently conveying his belief that technology can never entirely replace them.
Tom's Operation ... and After the Surgery
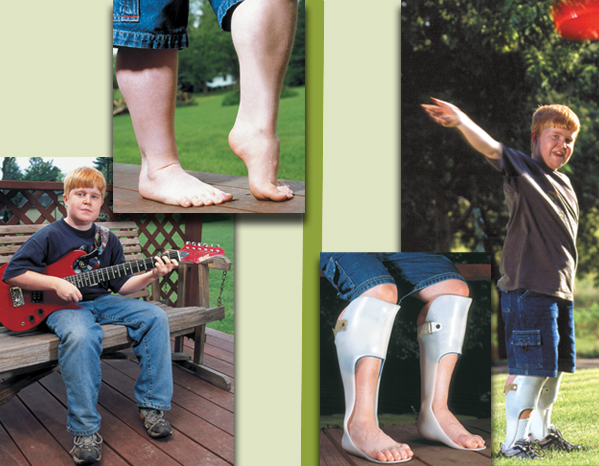
Left: Before the surgery, Tom Baker's heel cords (Achilles tendons) are contracted, pulling his feet — especially the left one — into an abnormal position and interfering with walking.
Right: A month after surgery, Tom's heels can once again reach the ground with ease. Plastic AFOs (ankle-foot orthoses) keep his ankles in the correct position for walking.
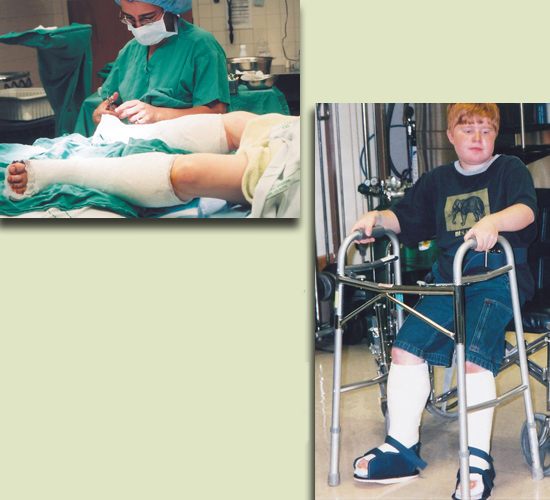
Left: In a short surgical procedure, Tom's heel cords are cut through stab wounds in each heel. Afterwards, while Tom is still under anesthesia, lower-leg casts are applied to keep his feet correctly positioned until braces can be made. Tom will wear the casts for a month.
Right: A few hours after his operation, Tom is already using a walker and cast shoes in the hospital's physical therapy department. His surgeon, Irwin Siegel, considers standing and walking right after surgery crucial to the operation's success.
MDA Resource Center: We’re Here For You
Our trained specialists are here to provide one-on-one support for every part of your journey. Send a message below or call us at 1-833-ASK-MDA1 (1-833-275-6321). If you live outside the U.S., we may be able to connect you to muscular dystrophy groups in your area, but MDA programs are only available in the U.S.
Request Information