Facioscapulohumeral Muscular Dystrophy (FSHD)
Signs and Symptoms
The onset, severity, and progression of facioscapulohumeral muscular dystrophy (FSHD) can vary widely. Most individuals develop symptoms in their teens or twenties, though some present in infancy. Muscle weakness typically begins in the face, shoulders, and upper arms, often in an uneven (asymmetric) pattern, and may gradually progress to other muscle groups.
In most people with FSHD, the disease progresses slowly. It can take as long as 30 years for symptoms to become seriously disabling, and not everyone reaches this stage. About 20% of people with FSHD eventually use a wheelchair at least part of the time.
Common Signs and Symptoms of FSHD
Facial weakness
Facial weakness is often the earliest sign of FSHD. It can make it difficult to smile, pucker the lips, whistle, or use a straw. Weakness typically affects the muscles around the eyes and mouth and may go unnoticed at first. Some individuals may also have difficulty fully closing their eyes during sleep.
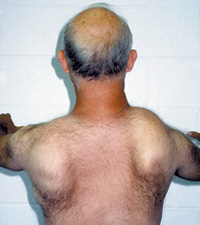
Shoulder weakness (scapular winging)
Weakness in the muscles that stabilize the shoulder blades is a hallmark of FSHD. This can cause the shoulder blades to protrude (scapular winging) and make it difficult to lift the arms overhead, throw objects, or reach for items. Weakness is often uneven between sides.
Lower leg weakness (foot drop)
Weakness in the muscles that lift the front of the foot can lead to “foot drop,” increasing the risk of tripping and difficulty walking, especially on stairs or uneven surfaces. Not all individuals are affected.
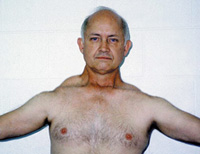
Abdominal weakness and posture changes
Weakness in abdominal muscles is common and may occur early. As it progresses, it can contribute to an exaggerated curve of the lower spine (lordosis), affecting posture and balance.
Hip (pelvic girdle) weakness
Some individuals develop weakness in the hips, often later in the disease. This can make it difficult to stand from a seated position, climb stairs, or walk long distances, and may lead to a waddling gait.
Pain and inflammation
Chronic pain is common in FSHD and may affect the shoulders, neck, lower back, and legs. Pain can result from muscle changes as well as strain related to posture and weakness.
Additional or Less Common Features
Joint and spinal changes
Muscle weakness can affect spinal alignment, sometimes leading to lordosis or mild scoliosis (side-to-side curvature of the spine).
Respiratory and cardiac involvement
Although many people with FSHD do not have significant breathing problems, respiratory involvement can be severe in some cases and may lead to serious complications. Monitoring of lung function may be recommended. Heart involvement is rare and usually mild, though periodic evaluation may be advised.
Eye (retinal) changes
Changes in the blood vessels of the retina are relatively common but rarely affect vision. Regular eye exams are recommended, especially in early-onset cases.
Hearing loss
Mild hearing loss can occur, particularly in individuals with childhood-onset FSHD. It is often subtle and detected through screening.
Swallowing difficulties (dysphagia)
Difficulty swallowing is rare but can occur due to weakness of facial and throat muscles.
Other Characteristics
Uneven (asymmetric) weakness
FSHD often affects one side of the body more than the other, sometimes noticeably. This asymmetry is a distinguishing feature of the disease.
Additional reading
- Preston MK, Wang LH. Facioscapulohumeral Muscular Dystrophy. 1999 Mar 8 [Updated 2025 Jul 10]. In: Adam MP et al., editors. GeneReviews® [Internet]. Seattle (WA): University of Washington, Seattle; 1993-2026. Available from: https://www.ncbi.nlm.nih.gov/books/NBK1443/
Last reviewed April 2026.

