Inclusion-Body Myositis (IBM)
Inclusion-Body Myositis (IBM)
What is inclusion body myositis (IBM)?
 Inclusion body myositis (IBM) is one of the idiopathic inflammatory myopathies (IIMs), a group of muscle diseases that involves inflammation of the muscles or associated tissues. The IIMs are sometimes referred to as simply “myositis.” It has become clear, however, that many forms of myositis exist. In IBM, inflammatory immune cells invade the muscle tissue and concentrate between the muscle fibers. These immune cells are recruited to and surround “inclusion bodies,” which contain cellular material from dead tissue. IBM is distinct among the IIMs for the presence of these inclusion bodies, which can be seen by muscle biopsy. It is estimated that approximately 20,000 people in the United States (US) have IBM, though the exact prevalence is unknown.
Inclusion body myositis (IBM) is one of the idiopathic inflammatory myopathies (IIMs), a group of muscle diseases that involves inflammation of the muscles or associated tissues. The IIMs are sometimes referred to as simply “myositis.” It has become clear, however, that many forms of myositis exist. In IBM, inflammatory immune cells invade the muscle tissue and concentrate between the muscle fibers. These immune cells are recruited to and surround “inclusion bodies,” which contain cellular material from dead tissue. IBM is distinct among the IIMs for the presence of these inclusion bodies, which can be seen by muscle biopsy. It is estimated that approximately 20,000 people in the United States (US) have IBM, though the exact prevalence is unknown.
What are the symptoms of IBM?
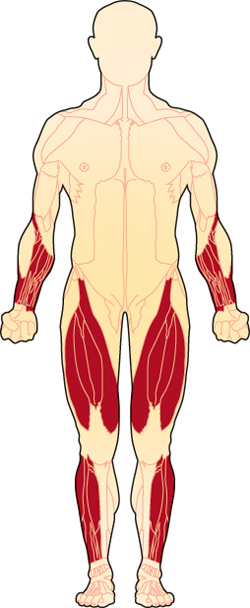
IBM causes progressive weakness of the muscles of the wrists and fingers, the muscles of the front of the thigh, and the muscles that lift the front of the foot. For more, see Signs and Symptoms.
What causes IBM?
The cause of idiopathic inflammatory myopathies like IBM is unclear. The body’s immune system turns against its own muscles and damages muscle tissue in an autoimmune reaction. The cause of the muscle degeneration that occurs in IBM is unclear as well. For more, see Causes/Inheritance.
What is the progression of IBM?
IBM usually develops after age 50 and is more likely to affect men than women. The disease progresses at different rates and with different symptoms in each person, but does not typically affect life expectancy. People with IBM may, however, experience persistent symptoms that require constant management over the course of a lifetime.
What is the status of research on IBM?
Research studies to increase the understanding of IBM and clinical trials of medications to treat IBM are underway. For a list of inclusion body myositis clinical trials, see MDA's Clinical Trials Finder Tool.
References
- Greenberg SA. Inclusion body myositis: clinical features and pathogenesis. Nat Rev Rheumatol. 2019;15(5):257-272. doi:10.1038/s41584-019-0186-x
- Naddaf E. Inclusion body myositis: Update on the diagnostic and therapeutic landscape. Front Neurol. 2022;13:2236. doi:10.3389/FNEUR.2022.1020113/BIBTEX
Last update: Feb 2023
Reviewed by Julie Paik, MD, MHS; Johns Hopkins University

