Becker Muscular Dystrophy (BMD)
Becker Muscular Dystrophy (BMD)
What is Becker muscular dystrophy?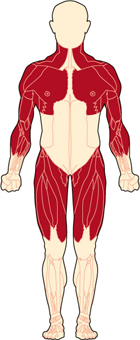
Becker muscular dystrophy affects the muscles of the hips, pelvic area, thighs, and shoulders, as well as the heart. Becker muscular dystrophy (BMD) is one of nine types of muscular dystrophies, a group of genetic, degenerative diseases primarily affecting voluntary muscles. BMD belongs to a group of dystrophinopathies including Duchenne muscular dystrophy (DMD) and an intermediate form between DMD and BMD. The disease is named after German doctor Peter Emil Becker, who first described this variant of DMD in the 1950s. BMD is similar to DMD but allows the voluntary muscles to function better than they do in DMD. BMD has a later onset and milder symptoms compared to DMD. The heart muscle, however, can be affected similarly to the way it can be in DMD.
What are the symptoms of BMD?
BMD's onset varies widely from 5 to 60 years of age,1 and the course is slower and less predictable than that of DMD. Generalized weakness first affects muscles of the hips, pelvic area, thighs, and shoulders. Calves are often enlarged. There can be significant heart involvement. For more, see Signs and Symptoms.
What causes BMD?
Until the 1980s, little was known about the cause of any kind of muscular dystrophy. In 1986, MDA-supported researchers identified the gene that, when flawed — a problem known as a mutation — causes DMD and BMD. In 1987, the protein associated with this gene was identified and named dystrophin.
Genes contain codes, or recipes, for proteins, which are important biological components in all forms of life. BMD occurs when the dystrophin protein that's made from a particular gene on the X chromosome is only partially functional.
The dystrophin protein keeps the muscle cell membrane from breaking or tearing when our muscles contract and relax. Because it connects the center of the muscle cell to the periphery, the dystrophin protein is extremely long. One end is specialized for linking to the muscle interior, and the other end for linking to a variety of proteins at the cell membrane. The long middle section, called the rod domain, is taken up by a series of repeating units called spectrin repeats.
The repeated spectrin units in the middle of the protein play an important role in linking the two ends, but the protein can still function (albeit not perfectly) with fewer of them than normal. Mutations that cause BMD decrease the number of these repeats, leading to muscle weakness.
In addition to its force-transfer role, dystrophin provides the scaffold for holding numerous molecules in place near the cell membrane. Loss of dystrophin displaces these molecules, with consequent disruptions in their functions.
While DMD mutations cause virtually no functional dystrophin to be made, people with BMD make dystrophin that is partially functional. They make a shortened form of the protein, which protects the muscles of those with BMD from degenerating as completely or as quickly as those of people with DMD.
BMD primarily affects boys and men, who inherit the disease through their mothers. Women can be carriers but usually exhibit no symptoms. For more about the way gene mutations cause BMD, see Causes/Inheritance.
What is life expectancy in BMD?
Most people with BMD survive well into mid to late adulthood. For more about living with BMD, see Medical Management. If the cardiac aspects of the disease are minimal, or if they are adequately controlled through medical intervention, a normal or nearly normal life span can be expected. Heart failure, due to a condition called dilated cardiomyopathy, is the main cause of death in BMD. Individuals living with BMD may have a near normal life expectancy, with some having an earlier death due generally to cardiac issues. In those patients the mean age of death was 47.3 with a range from 23-89.2
What is the status of BMD research?
Researchers are actively pursuing several strategies in BMD. Among the major strategies are gene replacement, gene modification, stem cell use, inhibiting a protein called myostatin, expanding the distribution and increasing the level of a protein called utrophin, and increasing blood flow to muscles.
MDA is supporting research in several of these areas. Human trials are underway for some of these strategies. For details, see Research.
Download our Becker Muscular Dystrophy (BMD) Fact Sheet
References
- Bradley, W. G., Jones, M. Z., Mussini, J. -M & Fawcett, P. R. W. Becker-type muscular dystrophy. Muscle Nerve (1978). doi:10.1002/mus.880010204
- Bushby KM, Gardner-Medwin D. The clinical, genetic and dystrophin characteristics of Becker muscular dystrophy. I. Natural history. J Neurol. 1993;240(2):98-104.
Last update: September 2024
Reviewed by Sumit Verma, MD; Emory University School of Medicine

